Your doctor will most likely ask about your medical history and menstrual cycles. You may be asked to keep a diary of bleeding and nonbleeding days, including notes on how heavy your flow was and how much sanitary protection you needed to control it.
Your doctor will do a physical exam and may recommend one or more tests or procedures such as:
Blood tests. A sample of your blood may be evaluated for iron deficiency (anemia) and other conditions, such as thyroid disorders or blood-clotting abnormalities.
Pap test. In this test, cells from your cervix are collected and tested for infection, inflammation or changes that may be cancerous or may lead to cancer.
Endometrial biopsy. Your doctor may take a sample of tissue from the inside of your uterus to be examined by a pathologist.
Ultrasound. This imaging method uses sound waves to produce images of your uterus, ovaries and pelvis.
Based on the results of your initial tests, your doctor may recommend further testing, including:
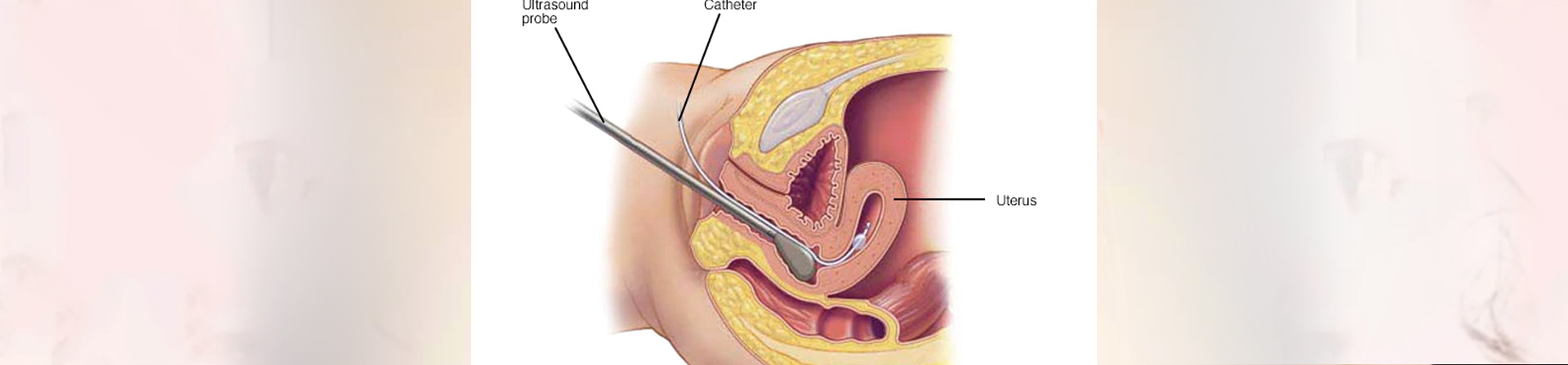
Sonohysterography. During this test, a fluid is injected through a tube into your uterus by way of your vagina and cervix. Your doctor then uses ultrasound to look for problems in the lining of your uterus.
Hysteroscopy. This exam involves inserting a thin, lighted instrument through your vagina and cervix into your uterus, which allows your doctor to see the inside of your uterus.
Doctors can be certain of a diagnosis of menorrhagia only after ruling out other menstrual disorders, medical conditions or medications as possible causes or aggravations of this condition.
Copyright ©2018 Shopweb All Rights Reserved